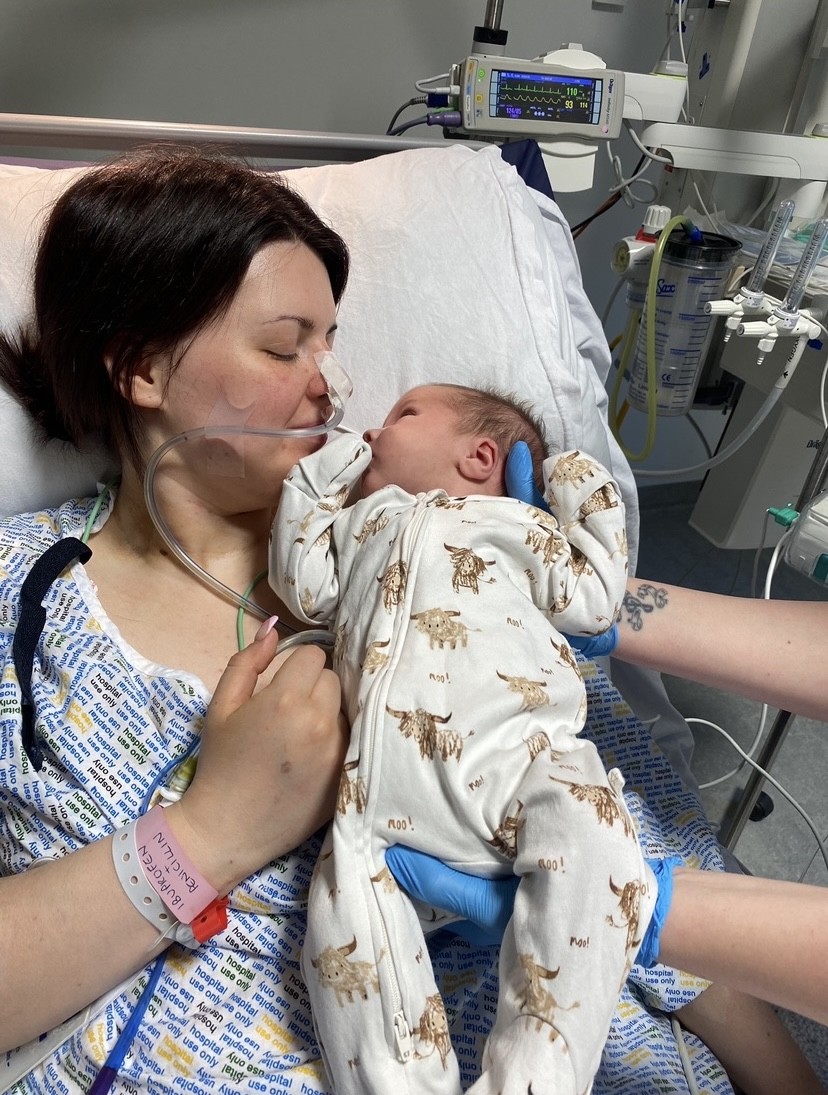
After developing a serious infection following a C-section, Michelle Gilchrist was repeatedly dismissed by healthcare professionals.
A photo of her maternity pad ultimately saved her life, leading to a sepsis diagnosis, emergency surgery, and weeks in hospital.
Single parent Michelle Gilchrist, 27, from Fife, is a mum of two young boys Rowan and Ruben aged 15 months and 18 weeks. But she nearly didn’t live to see them grow up.
After developing a life-threatening infection following her C-section, Michelle was dismissed by medical staff multiple times despite repeated complaints of worsening pain. It wasn’t until she showed a photograph of her maternity pad that a doctor finally listened and sent her for an emergency scan.
She was diagnosed with sepsis, and hours later underwent major life-saving surgery.
Michelle was first admitted to hospital for a planned C-section in April 2025. After giving birth, she quickly began experiencing severe burning abdominal pain. Despite raising her concerns several times, she was told the discomfort was “normal” and attributed to her recent surgery.
“I’d had a C-section the year before and I knew this pain was different,” Michelle said. “But no one would listen. My infection markers were raised, I was in agony and at one point I was pacing the floor at 4am asking for pain relief. A midwife refused me oramorph and said, ‘If you want to go home soon, we can’t give you that.’”
Michelle was discharged home after being given IV antibiotics, but continued to feel extremely unwell. She says she begged staff to recheck her infection levels before discharge but was told there was “no need”.
At home, her stomach pain got worse. She began experiencing breathlessness, heart palpitations, severe muscle pain and extreme shivering, despite also feeling clammy and sweaty.
“Even when I phoned the hospital and told them my symptoms, I had taken my temp at home which was 38.6, my blood pressure was 146/98 and my pulse was 132, I told them all this on the phone, I was told, “You could come in and get checked if you want to but they would probably just send you home again”. I was annoyed at this because I knew they weren’t taking my symptoms seriously and yet again weren’t listening to me, but I still went in because I knew something was wrong,” Michelle said.
No one took her seriously… until she showed her consultant a photo of what she thought was old blood on her maternity pad.
“That photo saved my life. It turned out to be pus from an abscess that had burst inside me. The minute I showed her, she said it rang alarm bells and sent me straight for a CT scan,” Michelle explained.
The scan revealed a 13cm abscess at the bottom of her stomach, a blood clot on one side of her abdomen and a pool of blood on the other side. Michelle underwent an emergency laparotomy on 18th April, just 17 days after her C-section.
“I was told the operation would take anything from 30 mins to two hours but when they opened me up they realised that it was much more complex and serious than they thought – that’s when they realised the abscess had burst and perforated my bowel, so the obstetrics consultants had to phone the general surgeons to come and help, there were four surgeons doing my operation and the operation ended up taking roughly five hours,” said Michelle.
She was told to prepare for the possibility of waking up with a stoma, and potentially losing her ovary and fallopian tube. Although surgeons were thankfully able to avoid this, she required two blood transfusions, iron infusions, and a high dependency stay to stabilise her.
“I was terrified. I thought I was dying. I’ve never felt pain like it. The consultant came to see me and said, ‘I’m so sorry Michelle, I’ll never forgive myself.’ They knew they should have listened earlier,” Michelle said.
Michelle spent over three weeks in hospital. Her mum – who works in hospital admissions – took time off work to look after Michelle and her sons.
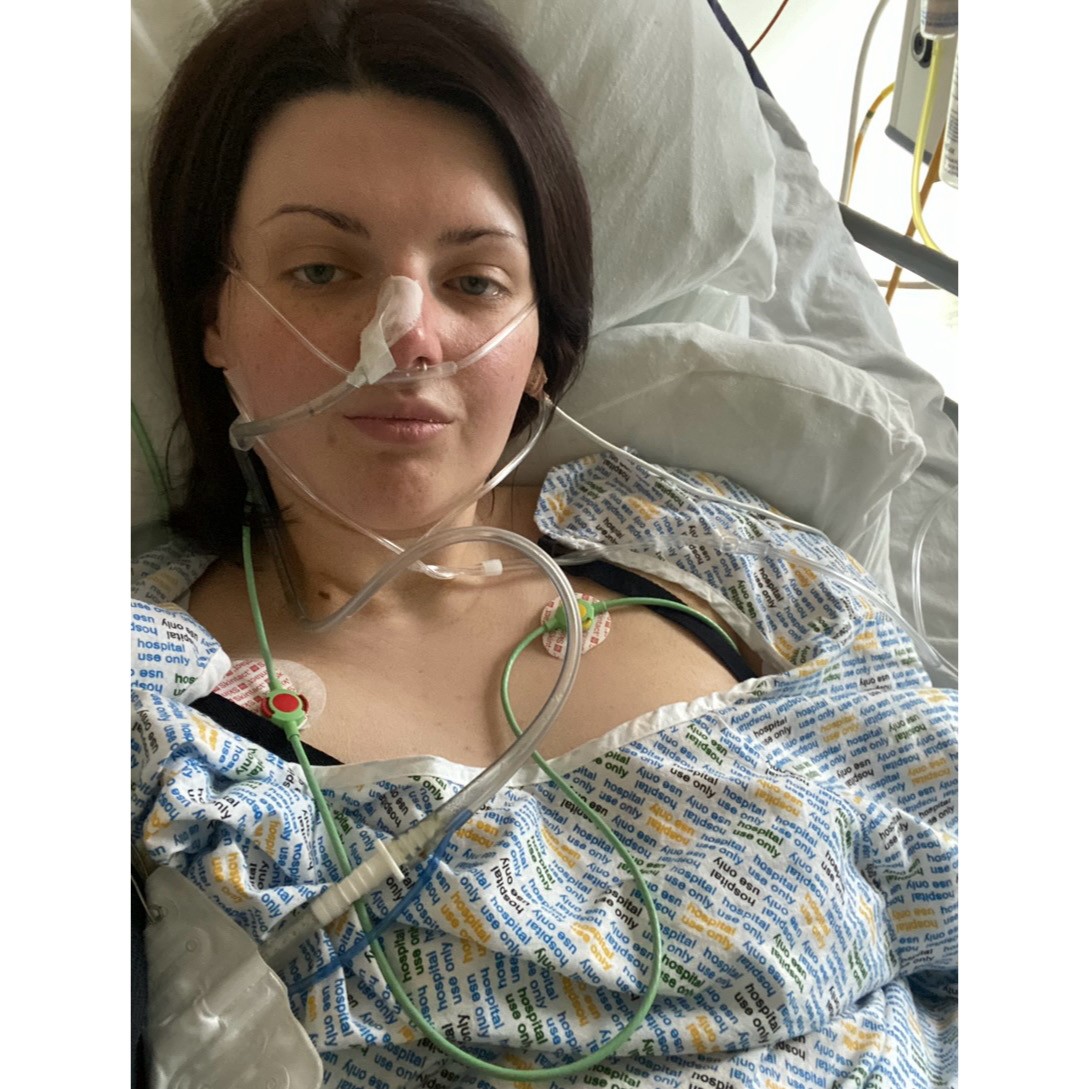
“I wasn’t allowed to eat for six days after my emergency laparotomy due to the injury of my bowel and was only allowed to sip water and orange juice for a week after with the help from the nurses/midwifes. It was horrendous. I lost all independence, I couldn’t do anything for myself for a long time, I remember waking up in high dependency absolutely screaming in pain when they were trying to turn me with a slide sheet. I had a drain in my stomach, a NG tube, oxygen, a PCA (morphine pump). I didn’t even know my newborn really for roughly the first six weeks of his life, it was heartbreaking. I couldn’t hold him, feed him or do anything for him. It’s all such precious time that I’ll never get back,” Michelle said.
A particularly difficult moment came when Michelle was told she had to stop breastfeeding due to the strength of the antibiotics she was on.
“My whole birth and breastfeeding journey was ruined by all of this. It’s been a horrific few months. I’ve been told if I was to ever have another birth, it would be life-threatening. Having that choice taken away from me has been soul-destroying, especially after missing all of the newborn stage with Ruben and knowing I’ll never get to experience it again. It’s something I’ve really struggled to come to terms with, especially with still being young,” Michelle said.
There are also physical reminders of her time in hospital.
“There is vein damage but it’s not permanent, but I’ve got loads of scar tissue in my arms from all the canulas and everyone’s still struggling to get my bloods because the veins are so damaged. They said the scar tissue in my arms might never go away,” said Michelle.
“An obstetrics consultant told me it would take probably 6 months to even start to feel “normal again” and around two years for my stomach to physically heal. I was told how slow and hard the recovery would be but I never thought for a second it would be this tough. I’m constantly wanting to do more than my body’s allowing me to. I’m constantly so weak, exhausted and in so much pain. It’s frustrating and hard to come to terms with. All the plans I had with my little boys for the summer have completely gone out the window,” she added.
She continues to suffer the effects of post-sepsis syndrome. She lives with daily exhaustion, poor mobility and nerve pain, and has been diagnosed with PTSD.
She attends nurse appointments twice a week for dressings, continues to attend appointments with multiple specialists, and take antibiotics.
“I had to learn to walk again. My stomach has been stitched badly, and I’ve been told any future abdominal surgery could be life-threatening. I missed my older son’s first birthday while I was in hospital – they kept telling me he wouldn’t remember, but that’s not what I needed to hear,” Michelle said.
Michelle says her GP has been her “rock”; she was left chasing her own follow-up care after being discharged without any support.
She wants to raise awareness of how easily sepsis can be missed, and the harm that can come from healthcare professionals dismissing patient concerns.
“They told me it was rare and I was hours from death. But if they’d just listened from the start, it could have been caught earlier with IV antibiotics and none of this would have happened. I knew something wasn’t right, and they kept blaming it on my health anxiety,” she said.
She urges others to trust their instincts and seek urgent medical advice if they suspect something is wrong.
“You know your own body better than anyone. If I hadn’t trusted my gut and taken that photo, I wouldn’t be here. I feel so lucky to be alive – and to still be here for my boys,” said Michelle.